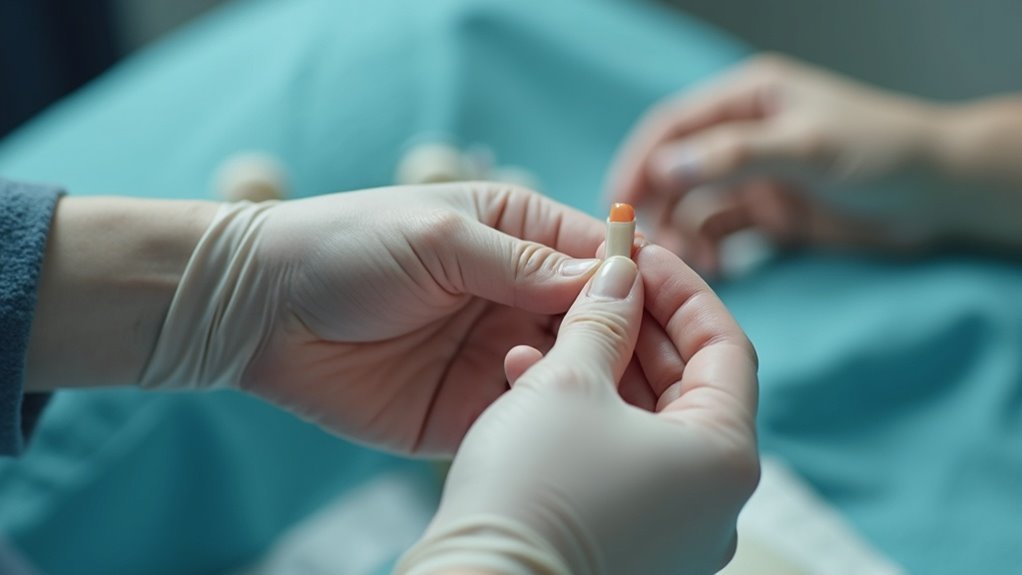
To set a dislocated finger safely in a survival situation, first reassure the injured person and help them find a comfortable position. If you have the means, administer a digital nerve block for pain relief. Carefully stabilize the proximal phalanx while gently pulling on the middle phalanx to disengage the dislocation. Align the middle phalanx with the proximal one, then extend the finger to complete the reduction. After the adjustment, assess for pain, range of motion, and stability to ensure proper healing. Follow up with effective splinting techniques to promote recovery. Remember, being prepared with knowledge on handling injuries can be crucial in emergency scenarios.
Key Takeaways
- Educate the individual about the reduction procedure to alleviate anxiety and ensure comfort during the process, emphasizing the importance of staying calm in survival situations.
- Use available supplies for pain management, such as a digital nerve block, if necessary, to enhance comfort while preparing for potential emergencies.
- Stabilize the proximal phalanx while gently pulling the middle phalanx to disengage the dislocated position, ensuring that the finger is realigned properly for effective use in survival scenarios.
- Extend the finger during the reduction to facilitate proper positioning and realignment of the joint, which is crucial for maintaining functionality in the field.
- After reduction, assess range of motion and monitor for potential complications like swelling or instability, as these can hinder survival efforts if not addressed promptly.
Understanding Finger Dislocations
Finger dislocations can pose significant challenges, not only affecting hand function but also impacting your ability to perform essential tasks during emergencies or survival situations.
These injuries can occur at various joints, with volar dislocations of the PIP joint in the fifth finger being particularly rare yet critical to assess. Symptoms include visible deformity, swelling, pain, and limited range of motion, all of which can hinder your capacity to manage survival scenarios effectively.
In prepping, understanding basic first aid for such injuries is vital. For pain management during the reduction process, techniques like digital nerve blocks may be beneficial, though not always accessible in survival settings.
It’s crucial to evaluate the injury by checking lateral stability and tendon function, particularly the flexor digitorum tendons, to ensure no further complications arise, such as central slip injuries, which can complicate the dislocation and hinder your ability to perform necessary tasks.
Being prepared with knowledge of how to handle finger dislocations can help you maintain functionality in critical situations, ensuring you can continue to provide for yourself and your loved ones.
Preparing for Reduction
Once you’ve assessed the finger dislocation and identified its type, it’s time to prepare for the reduction in a survival or prepping scenario.
First, calmly inform the patient about the procedure to alleviate anxiety—keeping morale high is essential in survival situations. Consider administering a digital nerve block using the web space technique for effective pain management, if you have the necessary medical supplies on hand.
Gather essential materials, including a splint for post-reduction immobilization, any tools for the nerve block, and first aid supplies.
Position the patient comfortably in a secure location, and explain each step of the process to keep them informed. Ensure the area is well-lit and as clean as possible to promote safety and minimize complications—this is crucial when resources are limited.
With everything in place and your skills in action, you’re ready to proceed with the reduction technique, ensuring the patient is stabilized for whatever challenges lie ahead.
Reduction Technique Step-by-Step
As you prepare to perform the reduction in a survival situation, brace the proximal phalanx with one hand to provide counter traction, while your other hand grasps the middle phalanx. Apply gentle axial traction on the middle phalanx to disengage it from the dislocated position. While maintaining traction, carefully pull the middle phalanx back into alignment with the proximal phalanx, extending the finger to facilitate the reduction.
| Step | Action | Purpose |
|---|---|---|
| 1. Brace | Stabilize proximal phalanx | Provide counter traction |
| 2. Traction | Gently pull middle phalanx | Disengage dislocated position |
| 3. Alignment | Align middle with proximal phalanx | Restore normal positioning |
| 4. Extension | Extend finger | Aid in reduction process |
In emergency scenarios, knowing how to perform such techniques can be crucial for maintaining functionality and preventing further injury.
Post-Reduction Assessment
After successfully reducing a dislocated finger, it’s critical to assess its condition to ensure proper healing and functionality, especially in survival situations where injuries can impede your ability to perform essential tasks.
Start by checking the full range of motion, confirming that no pain or swelling restricts movement. Next, evaluate lateral stability and the flexor digitorum tendons by testing the flexor digitorum superficialis and profundus with specific maneuvers.
Begin by assessing motion and pain, then evaluate tendon stability through targeted tests for comprehensive recovery.
Conduct the Elson test to check for potential central slip injuries; instruct the individual to curl their fingers around a sturdy surface, applying pressure to the middle phalanx.
Lastly, keep an eye out for any signs of instability and consider scheduling regular follow-ups with a medical professional to ensure ongoing assessment and readiness for any survival challenges that may arise.
Treatment Protocols for Dislocated Fingers
When managing dislocated fingers in a survival situation, it’s crucial to apply the right treatment protocols based on the type of dislocation.
For volar dislocations, splint the finger in extension for three weeks to ensure proper alignment.
Dorsal and lateral dislocations may require specific splinting angles or buddy taping for two to three weeks to stabilize the injury.
In a prepping context, having a first-aid kit that includes splints and tape is essential.
Regular follow-ups with a medical professional, such as a hand surgeon, are important to monitor healing and prevent complications, especially when access to medical care may be limited.
Volar Dislocation Management
To effectively manage a volar dislocation at the PIP joint of the fifth finger, it’s crucial to approach this situation with a survival mindset. Here are the steps to follow:
- Assess for Injury: Before attempting any reduction, evaluate for potential injuries to the flexor digitorum tendons and lateral stability. This assessment is essential to ensure you aren’t compounding any injuries.
- Post-Reduction Check: After reduction, check the range of motion, stability, and tendon function. This step is vital in identifying any complications early on.
- Pain Management: Consider using digital nerve blocks for pain management during the reduction process. Employ the web space technique to effectively numb the area, which can be particularly helpful in a survival scenario where pain relief options are limited.
- Long-Term Care: Splint the finger in extension for three weeks to create an ideal healing environment.
Regular monitoring for potential complications such as central slip injuries is essential, especially in a survival situation where access to medical care may be limited.
Dorsal and Lateral Care
Proper care for dorsal and lateral dislocations of the fingers is essential, especially in survival situations where self-reliance is crucial.
For dorsal dislocations, it’s important to immobilize your finger in 30 degrees of flexion or utilize buddy taping for two to three weeks to ensure it heals correctly. In the wilderness, buddy taping can be a practical and effective method to stabilize the injury.
When dealing with lateral dislocations, similar buddy taping will provide the necessary support during your recovery.
Before any treatment, it’s vital to assess the stability of the joint and the function of the tendons. After reducing the dislocation, check for full range of motion, stability, and tendon function to ensure everything is aligned properly.
Regular follow-ups with a medical professional are crucial to monitor for any complications and to ensure that the injury heals correctly, especially when resources are limited in a survival scenario.
Importance of Follow-Up Care
Follow-up care is crucial for ensuring your readiness and resilience after an injury, such as a dislocated finger.
Regular assessments will help you monitor your healing progress and detect any complications early, which is vital for maintaining your ability to respond effectively in emergency situations.
Always prioritize attending scheduled medical appointments and be vigilant in reporting any unusual symptoms, as these could impact your overall preparedness and survival capabilities.
Monitor Healing Progress
Monitoring the healing progress of a dislocated finger is vital not just for recovery, but also for ensuring you’re fit for any survival situation. Regular follow-ups with your hand surgeon can help catch issues early.
Here are key aspects to focus on:
- Appointment Frequency: Schedule follow-ups within a week of the injury and continue every few weeks until healed. This ensures that any complications are addressed promptly, allowing you to maintain your preparedness.
- Functional Assessment: During each visit, evaluate your range of motion, stability, and overall functionality. In survival situations, being able to use your hands effectively is critical.
- Complication Awareness: Stay alert for signs of complications such as increased pain, swelling, or reduced mobility. These symptoms may require immediate medical attention and could impact your ability to handle emergency scenarios.
Adhering to splinting or buddy taping protocols is essential for optimal recovery, ensuring you remain capable and ready for any challenges that may arise.
Assess for Complications
How can you ensure your dislocated finger heals properly while preparing for survival situations?
First, assess for complications like central slip injuries using the Elson test to check tendon function. Schedule regular follow-ups with a skilled medic or hand specialist to monitor for stiffness, instability, or tendon injuries post-reduction.
After reduction, evaluate your finger’s full range of motion, documenting any pain or swelling that could impede recovery. During follow-ups, assess lateral stability to rule out ligamentous injuries.
Be aware that transient blood flow issues from digital nerve blocks may necessitate adjustments in pain management strategies.
Close observation and proper care are essential for a successful recovery, especially when preparing for emergencies where hand functionality is crucial.
Ensure Proper Functionality
Ensuring proper functionality after a dislocated finger is crucial, especially in survival situations where hand dexterity is essential. Regular follow-up care with a hand specialist is vital for monitoring complications and recovery.
- Stability Evaluation: Regular assessments are key to checking lateral stability and tendon function, ensuring your finger heals correctly and maintains its strength for survival tasks.
- Injury Detection: Tests like the Elson test can identify potential central slip injuries, which are crucial for maintaining functionality in high-stress scenarios.
- Range of Motion: Ongoing evaluation of motion and strength is important to detect long-term effects and guide rehabilitation, ensuring you remain capable in any situation.
Adhering to splinting or buddy taping protocols is essential for healing, so be sure to follow your specialist’s advice diligently for optimal recovery and readiness.